How has COVID-19 impacted patients living with chronic illness? Global survey results
Published 5 Oct 2021 • By Courtney Johnson
As we soon head into the second year of the COVID-19 pandemic, many are looking back at what we have learned from the virus. Throughout 2020, Carenity conducted a survey to understand the COVID-19 pandemic from the chronic illness patient perspective in partnership with Viatris and two associations dedicated to informal carers and their organisations: “La Compagnie des Aidants” and “Eurocarers”.
How has COVID-19 impacted patients’ daily lives, their access to care, and their disease management over the past year? What about their social and mental well-being?
Discover our findings below!

4,831 Carenity members participated in our COVID-19 survey across 6 country platforms
Our 2020 COVID-19 survey was organised in two waves: the first wave was conducted from 22 June – 14 August, 2020 and the second from 2 November – 29 December, 2020.
2,489 members participated in the first wave and 2,342 in the second, with 195 patients participating in both waves.
Participants came from the following countries:
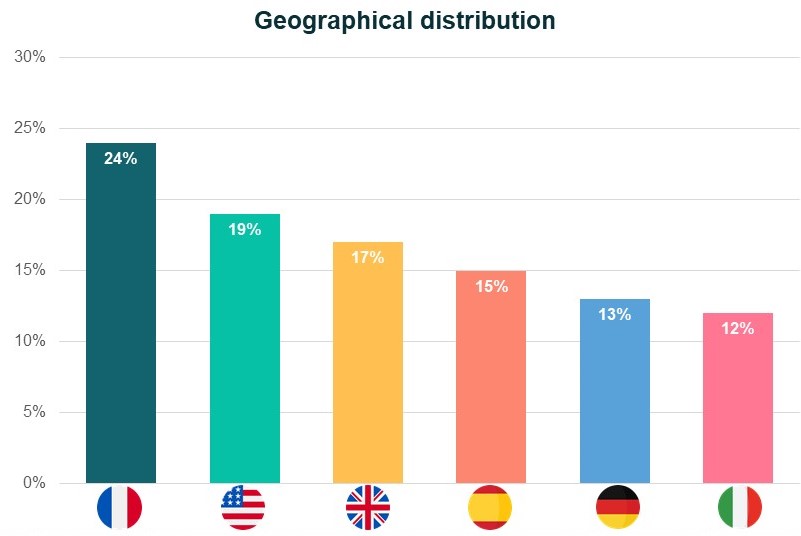
Across both waves of the survey, patients were mostly women (62%), with a mean age of 53 years old (in the summer of 2020) or 52 years old (in winter 2020).
The survey was focused on patients living with noncommunicable diseases, including metabolic diseases (diabetes, obesity...), chronic respiratory diseases (asthma, COPD...), mental health conditions (depression, anxiety, bipolar disorder...), cardiovascular diseases (heart failure, high blood pressure, stroke... ), and cancer.
Of those conditions, the most common conditions among patients were type 2 diabetes (30%), asthma (23%), high blood pressure (18%), chronic anxiety (14%), COPD (13%), and depression (13%). Many members had more than one chronic illness.
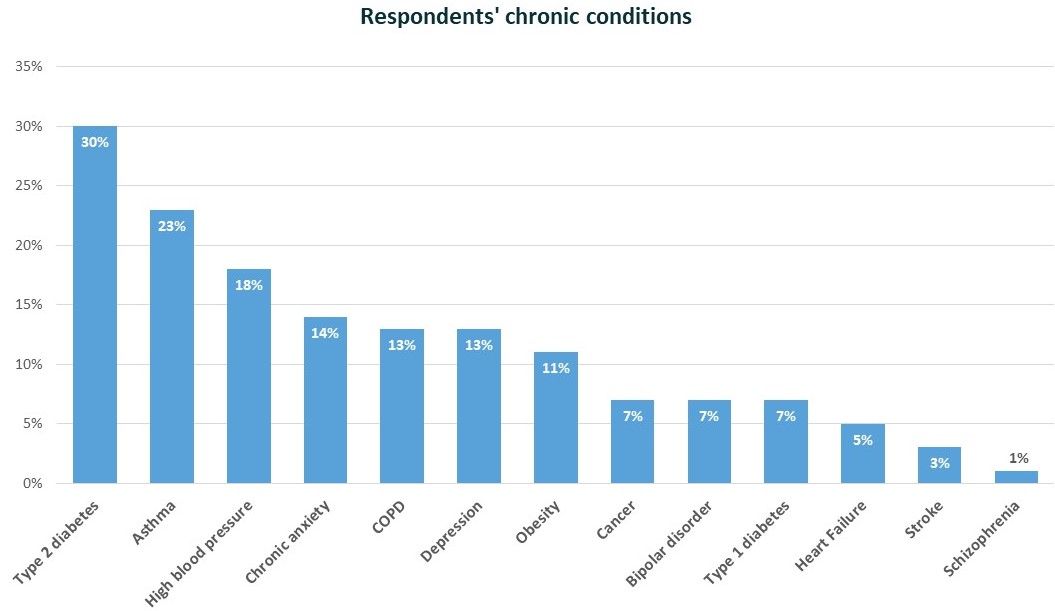 Patients' conditions, Nov-Dec 2020
Patients' conditions, Nov-Dec 2020
90% of respondents were taking a regular or long-term treatment for their health condition(s).
50% of patients surveyed experienced a worsening of their condition
When asked about how their condition had evolved during the different periods of COVID-19 lockdown, 1 in 2 patients surveyed reported that their condition had worsened.
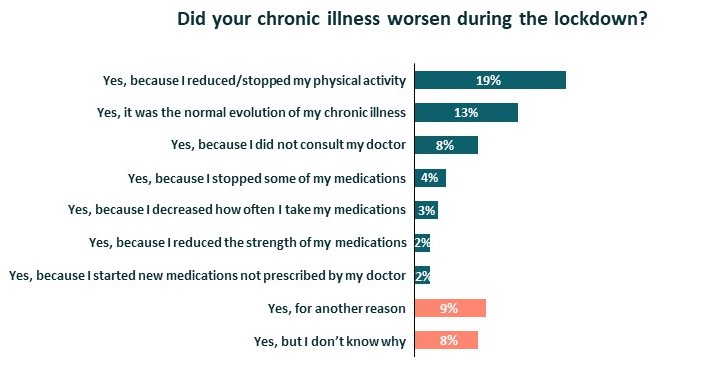
Of those patients, almost 20% attribute this worsening to their reduction or complete stoppage of physical activity, 13% to the normal progression of their illness, and 8% to having not been able to consult their physician.
17% of patients developed a new chronic condition during lockdown
Additionally, 17% of respondents indicated that they developed a new chronic health condition during the COVID-19 lockdown. Among these participants, 83% contacted a healthcare professional about it: their general practitioner, their specialist (pulmonologist, endocrinologist, etc.) or a healthcare professional in a hospital emergency centre. More specialists and pharmacists were contacted during the winter period.
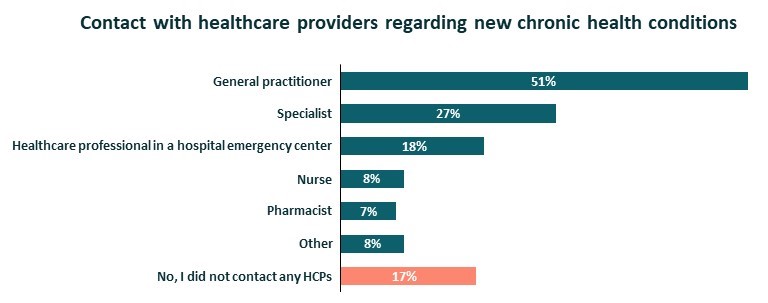 Patient contacts with HCPs, Jun-Aug 2020
Patient contacts with HCPs, Jun-Aug 2020
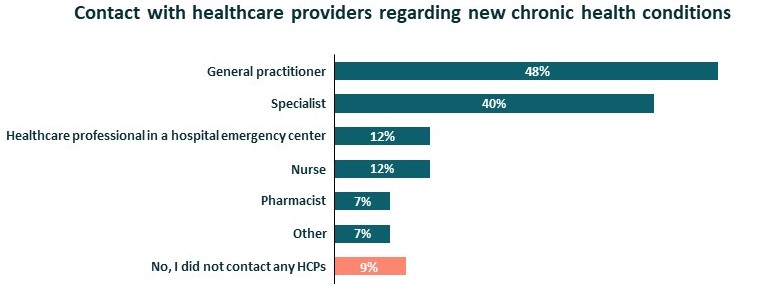 Patient contacts with HCPs, Nov-Dec 2020
Patient contacts with HCPs, Nov-Dec 2020
Access to care for chronic patients improved as the pandemic progressed
Fortunately, as the pandemic progressed and protective measures against COVID-19 were put in place, patients saw an overall improvement in their access to care as compared to at the start of the initial outbreak.
During the first wave of the survey in the summer of 2020 (from June to August), almost 40% of patients reported seeing their doctor less frequently than usual, 30% had trouble finding an available doctor, and 52% had their medical appointments or procedures cancelled or postponed.
By that winter (November to December), both patients’ frequency of consultation and number of postponed or cancelled medical visits or procedures had improved, while their difficulty in finding an available doctor remained stable.
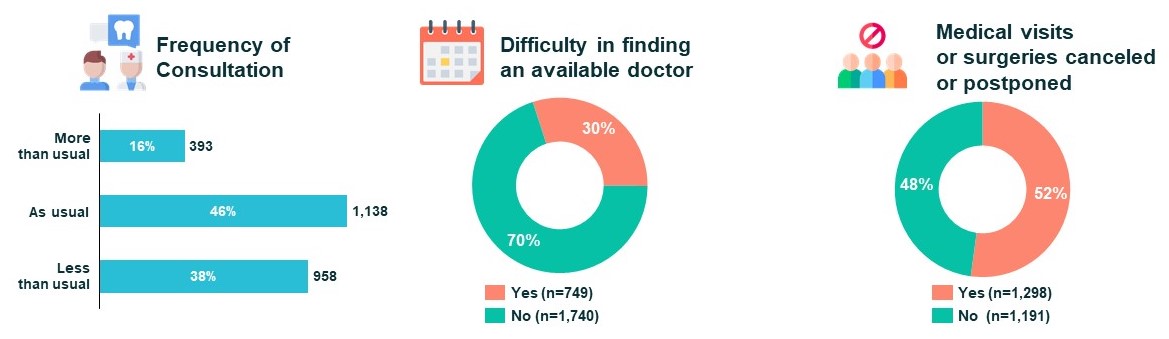
Patients’ access to care, Jun-Aug 2020
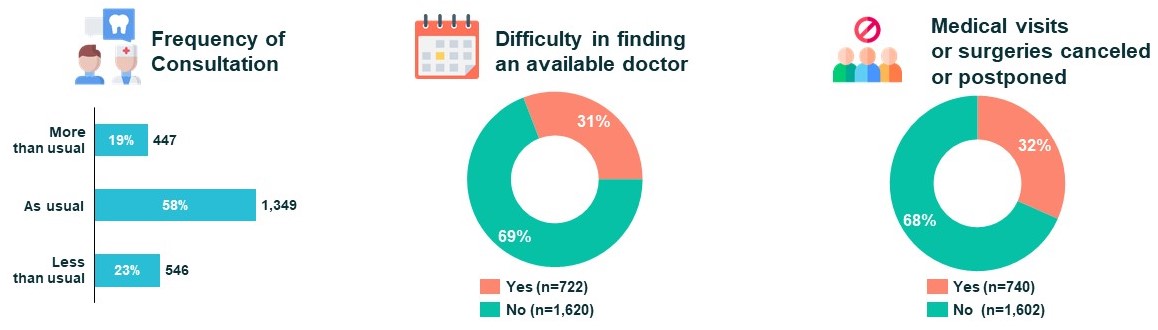
Patients’ access to care, Nov-Dec 2020
Similarly, patients taking regular or long-term treatments witnessed a similar improvement in access to their medications, with a 3% decrease in the number of patients having difficulty finding their treatment at the pharmacy.
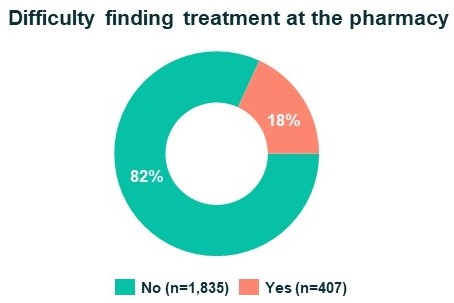
Patients’ access to treatment, Jun-Aug 2020
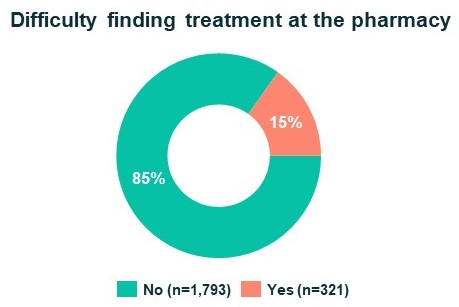 Patients’ access to treatment, Nov-Dec 2020
Patients’ access to treatment, Nov-Dec 2020
The COVID-19 pandemic has taken a toll on patients’ mental health
Patients experienced varying levels of social isolation throughout the pandemic. In the summer of 2020, 54% of patients across our 6 country platforms indicated that they felt very or completely isolated (rating their isolation between 6 and 10 out of 10). By winter 2020, this proportion decreased to 48% overall, but not to the same extent in each country.
Social isolation was higher for our member in the US and UK in both waves of the survey, but while UK members’ feelings of isolation decreased as the pandemic progressed, the opposite was true for those in the US:
Patients’ levels of social isolation, Jun-Aug 2020
Patients’ levels of social isolation, Nov-Dec 2020
These heightened levels of isolation took a toll on members’ stress and state of mind. Patients’ level of stress remained the same across the two waves for all countries except the United States, where stress increased.
Patients’ levels of stress, Jun-Aug 2020
Patients’ levels of stress, Nov-Dec 2020
Patients call for more information about their conditions and COVID-19
In the first wave of our survey, one third of all patients reported that they had received no information about their health condition and COVID-19.
Of those who did receive information about their condition in the context of COVID-19, 25% overall were unsatisfied with the quality of this information.
This access to information varied by country; in the United States, for example, 70% of patients were satisfied with the information they had received:
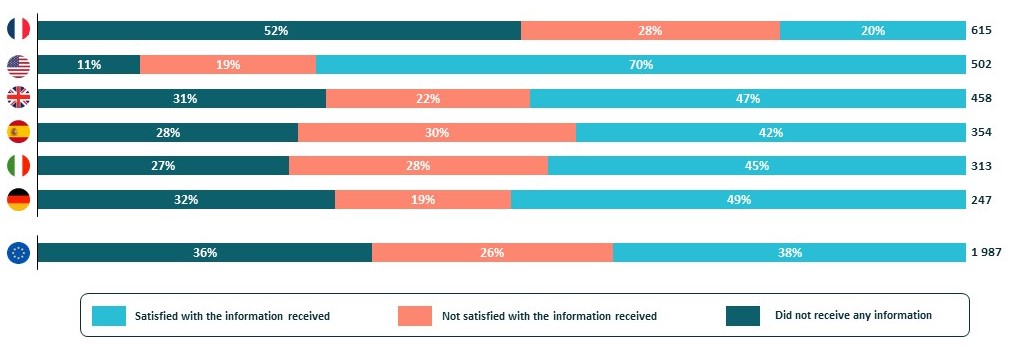 Patients’ satisfaction with information they received about their condition and COVID-19, Jun-Aug 2020
Patients’ satisfaction with information they received about their condition and COVID-19, Jun-Aug 2020
When asked what additional information they would have liked to have received, members particularly called for: information about the risks associated with their condition (59%), advice on how to deal with the end of the lockdown (32%), and information about available psychological support (29%):
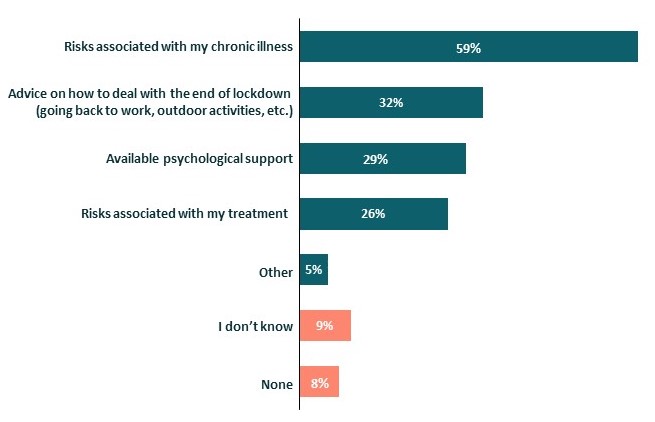 Additional information patients would have liked to have received, Jun-Aug 2020
Additional information patients would have liked to have received, Jun-Aug 2020
When asked about solutions or services that would be helpful to help members cope with the pandemic, quality information was by and large the most mentioned by patients. Respondents first wanted more information from health authorities and from the media.
After information, members looked to the comfort of their loved ones, wishing for unrestricted access to family and friends while in lockdown.
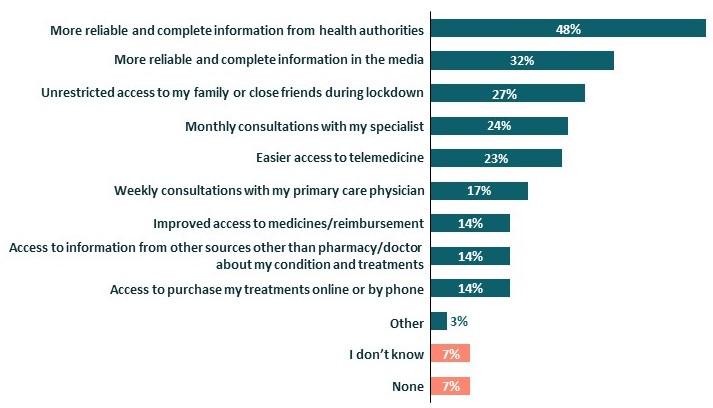
Additional solutions and services would have liked to cope with the COVID-19 pandemic, Jun-Aug 2020
And what about you? How has the COVID-19 pandemic impact your daily life?
Share your thoughts with the community in the comments below!
Take care!
Reference: Pécout C, Pain E, Chekroun M, Champeix C, Kulak C, Prieto R, van Vugt J, Gilchrist K, Lainé-Pellet AF. Impact of the COVID-19 Pandemic on Patients Affected by Non-Communicable Diseases in Europe and in the USA. Int J Environ Res Public Health. 2021 Jun 22;18(13):6697. doi: 10.3390/ijerph18136697. PMID: 34206293; PMCID: PMC8297015. https://www.mdpi.com/1660-4601/18/13/6697/htm
About Viatris 
Viatris Inc. (NASDAQ: VTRS) is a new kind of healthcare company, empowering people worldwide to live healthier at every stage of life. We provide access to medicines, advance sustainable operations, develop innovative solutions and leverage our collective expertise to connect more people to more products and services through our one-of-a-kind Global Healthcare Gateway®. Formed in November 2020, Viatris brings together scientific, manufacturing and distribution expertise with proven regulatory, medical and commercial capabilities to deliver high-quality medicines to patients in more than 165 countries and territories. Viatris' portfolio comprises more than 1,400 approved molecules across a wide range of therapeutic areas, spanning both non-communicable and infectious diseases, including globally recognized brands, complex generic and branded medicines, a growing portfolio of biosimilars and a variety of over-the-counter consumer products. With a global workforce of more than 40,000, Viatris is headquartered in the U.S., with global centres in Pittsburgh, Shanghai and Hyderabad, India. Learn more at viatris.com and investor.viatris.com, and connect with us on Twitter at @ViatrisInc, LinkedIn and YouTube.
About La Compagnie des Aidants 
La Compagnie des Aidants (CDA), founded in 2009 by Claudie KULAK, is a non-profit organisation with the goal of providing support to carers in many significant areas . More specifically, CDA aims to provide a wide range of tools and information [training, advice, network (who’s who)], raise awareness of the significant contribution made by carers to care recipients' life and health, in household organisation and all aspects of daily life, lead advocacy activities towards public authorities for ensuring that national policies take carers into account. The main activities include networking (the directory “who’s who” allows cares to get to know each other, to exchange information, to fight against social exclusion and loneliness), online training (20 online tutorials on gestures/postures and emotional relationship with the care recipient have been produced) and the awareness campaign the “French caravan tour” (in 2021, 30 cities visited – the caravan parks 3 days outside of hospitals, shopping centres or public places to meet informal carers and answer their questions). La Compagnie des Aidants is also part of the French Economic and Social Committee. For more information: https://lacompagniedesaidants.org/
About Eurocarers 
Eurocarers brings together 75 carers’ organisations as well as relevant universities & research institutes from 26 countries. Our network works to ensure that care is valued, and unpaid care is recognized as central to the sustainability of health and long-term care systems. Eurocarers acts as a voice for informal carers, irrespective of their age or the particular health and care need of the person they are caring for. For more information: https://eurocarers.org/
5 comments


 Facebook
Facebook Twitter
Twitter




